Is obesity simply a result of lifestyle choices, or is it something deeper—a disease that affects how your body works? You might think losing weight is just about eating less and moving more, but what if there’s more happening inside your body that makes shedding pounds a real challenge?
Understanding whether obesity is a disease could change how you see your health and the solutions available to you. You’ll discover surprising facts about obesity, why it’s not just about willpower, and what this means for your journey toward better health.
Keep reading to uncover the truth that might just transform your approach to weight and wellness.
Obesity As A Disease
Obesity is a complex condition affecting millions worldwide. It involves excess body fat that harms health. The question remains: is obesity a disease? This topic sparks much discussion among doctors, scientists, and the public. Understanding obesity as a disease helps clarify its causes and treatments.
Medical Classifications
Many health organizations classify obesity as a disease. The Centers for Disease Control and Prevention (CDC) officially labels obesity as a chronic disease. The World Health Organization (WHO) also recognizes obesity as a medical condition. This classification helps guide treatment plans and insurance coverage. It highlights that obesity is not just about weight but involves biological changes. Obesity affects metabolism, hormones, and inflammation in the body. These changes make weight loss difficult to maintain without medical support.
Debates And Perspectives
Not everyone agrees on calling obesity a disease. Some experts argue obesity is a risk factor for other diseases, not a disease itself. They say obesity results from lifestyle choices like diet and exercise. Others believe calling obesity a disease reduces stigma and promotes better care. It shifts focus from blame to medical treatment. This view supports using medications and surgery when needed. The debate continues as research reveals more about obesity’s causes. Understanding these perspectives helps improve support for those affected.

Credit: drharshsheth.com
Biological Factors
Biological factors play a crucial role in understanding obesity. They explain why some people gain weight more easily. These factors involve complex changes inside the body. They affect metabolism, hormones, and genetics. This section explores these biological aspects in detail.
Metabolic Changes
Metabolism controls how the body uses energy. In obesity, metabolic changes often occur. The resting metabolic rate may slow down. This means fewer calories are burned at rest. The body adapts to dieting by conserving energy. This makes weight loss harder to achieve. Metabolic changes can also affect how fat is stored.
Hormonal Imbalances
Hormones regulate hunger and fullness signals. Leptin is one key hormone that signals when to stop eating. In obesity, leptin resistance can develop. The brain no longer gets the fullness signal. Hunger hormones like ghrelin may increase, causing more appetite. Low thyroid hormone levels can slow metabolism. These imbalances create a strong drive to eat more.
Genetic Influences
Genes affect how the body stores and burns fat. Some people inherit genes that increase obesity risk. These genes can influence appetite and metabolism. Genetic predispositions make weight control more difficult. They do not guarantee obesity but raise the chances. Understanding genetics helps explain why obesity is complex.
Physiological Challenges
Obesity involves complex physiological challenges that affect the body’s ability to maintain a healthy weight. These challenges make weight loss difficult and often require more than just diet and exercise. Understanding these factors helps explain why obesity is recognized as a disease by many health experts.
Leptin Resistance
Leptin is a hormone that tells the brain when the body has enough fat stored. In obesity, the body becomes less sensitive to leptin. This means the brain does not get the signal to stop eating. People with leptin resistance may feel hungry even with excess fat. This disrupts normal appetite control and leads to overeating.
Metabolic Adaptation
The body’s metabolism can slow down during weight loss efforts. This is called metabolic adaptation. It means fewer calories are burned at rest. The body tries to conserve energy by lowering the metabolic rate. This makes it harder to lose weight and easier to regain it. Metabolic adaptation can last for a long time.
Chronic Inflammation
Obesity causes chronic low-level inflammation in the body. Fat tissue releases substances that trigger this inflammation. It can affect how the body uses insulin and other hormones. Chronic inflammation contributes to insulin resistance and other health problems. It also makes losing weight more challenging.
Lifestyle And Environmental Effects
Obesity is influenced by many lifestyle and environmental factors. These elements shape how the body stores fat and responds to food. Understanding these effects helps explain why obesity is complex and not just about overeating.
Daily habits, surroundings, and health conditions all play roles. They affect metabolism, hunger signals, and the ability to lose weight. The body’s response to these factors can make managing weight very challenging.
Sleep And Stress
Poor sleep disrupts hormones that control hunger and fullness. Lack of rest raises levels of ghrelin, the hunger hormone, causing overeating. Stress triggers cortisol release, which promotes fat storage, especially around the belly. Chronic stress can also lead to emotional eating and less physical activity.
Medications Impact
Some medications cause weight gain as a side effect. Antidepressants, antipsychotics, and steroids often increase appetite or slow metabolism. These drugs can alter how the body stores and uses energy. This makes weight management harder for people taking them.
Weight Loss History
Repeated dieting can slow down metabolism over time. The body adapts to fewer calories by burning less energy at rest. This “metabolic adaptation” makes future weight loss more difficult. Many people regain weight quickly after losing it, creating a cycle that affects health.
Treatment Approaches
Treating obesity requires multiple approaches tailored to individual needs. Effective treatment often combines surgery, medication, and behavioral changes. Each method targets different aspects of obesity to improve health and quality of life.
Bariatric Surgery
Bariatric surgery helps reduce stomach size to limit food intake. It also changes hormone levels that affect hunger and fullness. This surgery suits people with severe obesity who have not succeeded with other methods. It can lead to significant and lasting weight loss. Surgery also lowers risks of diabetes, heart disease, and other conditions.
Medications For Weight Loss
Medications support weight loss by controlling appetite or reducing fat absorption. Doctors prescribe these drugs for patients with obesity and related health problems. They work best when combined with diet and exercise. Medications can help overcome biological factors that make weight loss hard. Side effects may occur, so medical supervision is essential.
Behavioral Interventions
Behavioral changes focus on diet, physical activity, and habits. Counseling helps people understand triggers for overeating and develop coping skills. Small, consistent changes often lead to better results than drastic diets. Support groups and therapy provide motivation and accountability. These interventions address emotional and psychological aspects of obesity.

Credit: www.medkart.in
Social And Psychological Dimensions
The social and psychological aspects of obesity shape how society views this condition. These dimensions affect the lives of those living with obesity beyond the physical health risks. Understanding these factors is key to addressing obesity in a compassionate and effective way.
Social attitudes and mental health challenges often intertwine with obesity. The experience of stigma and the presence of mental health issues can worsen the impact of obesity. These factors also influence how people seek and receive care.
Stigma And Misconceptions
Many people with obesity face stigma in daily life. They may be judged unfairly as lazy or lacking willpower. These misconceptions ignore the complex causes of obesity.
Stigma can lead to social isolation and lower self-esteem. It can also discourage individuals from visiting doctors or joining weight-loss programs. This social barrier makes managing obesity harder.
Public education is needed to reduce stigma. Emphasizing obesity as a medical condition helps change negative views. Respectful language and understanding create a more supportive environment.
Mental Health Factors
Mental health plays a crucial role in obesity. Depression, anxiety, and stress are common among those affected. These conditions can lead to emotional eating or reduced physical activity.
Obesity itself can increase the risk of mental health disorders. The cycle between obesity and mental health issues can be hard to break. Treatment should address both physical and psychological needs.
Support from counselors or therapists helps improve mental well-being. Combining mental health care with medical treatment leads to better outcomes. Recognizing this connection is vital in managing obesity effectively.
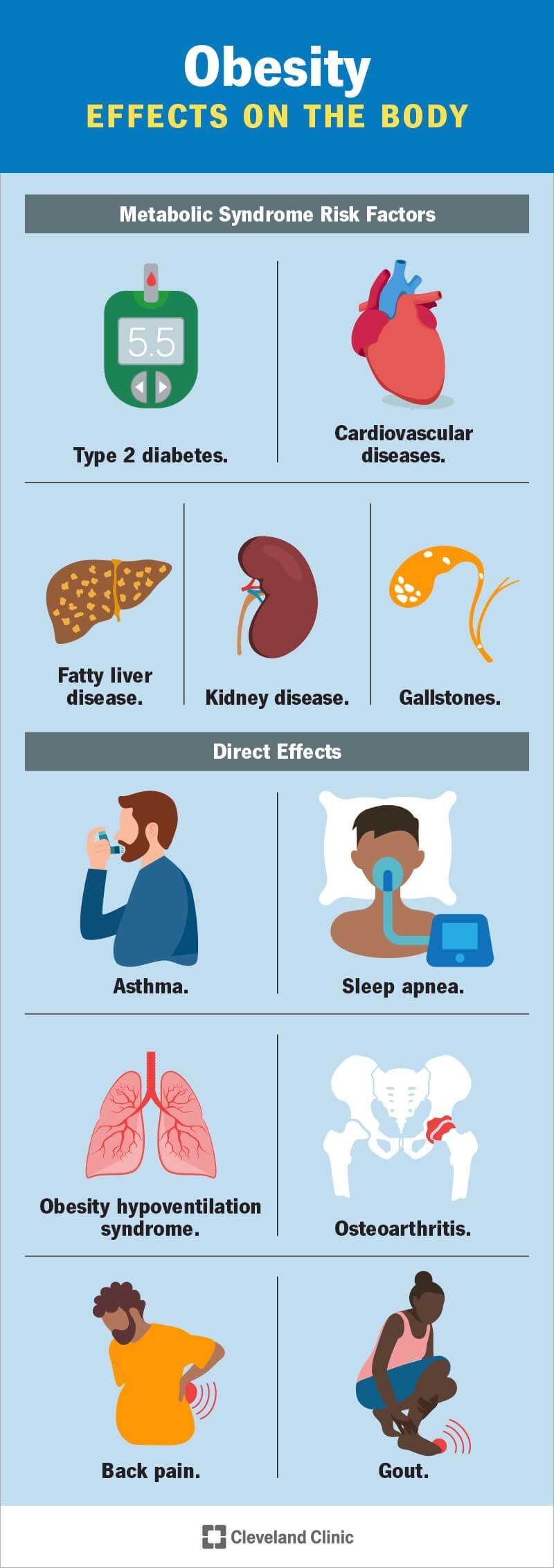
Credit: my.clevelandclinic.org
Conclusion
Obesity affects millions worldwide and impacts overall health deeply. Many health groups label obesity as a disease due to its complex causes. It involves genetics, hormones, and metabolism, not just lifestyle choices. Understanding obesity as a disease can lead to better care and support.
Treating it requires patience, medical help, and healthy habits. Recognizing obesity’s nature helps reduce stigma and encourages empathy. Everyone deserves respect and proper treatment regardless of their weight. Addressing obesity with knowledge brings hope for healthier lives ahead.

